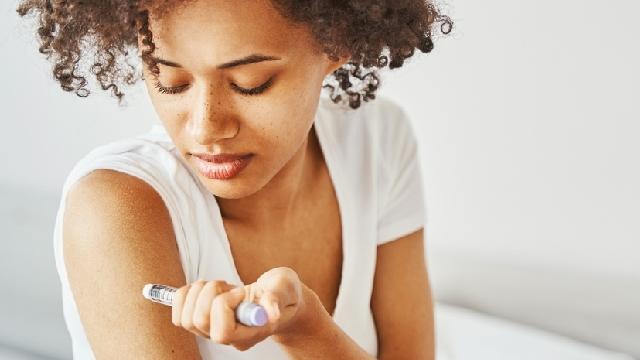
Insulin and diabetes
Everyone with type 1 diabetes needs to take insulin as a medication. And so do some people with type 2 diabetes, some people with gestational diabetes and some people with other types of diabetes.
Insulin helps you manage your blood sugar levels and helps prevents short-term or long-term serious health problems known as diabetes complications.

What is insulin resistance?
Find out what insulin resistance is and what it means for your type of diabetes - or risk of diabetes.
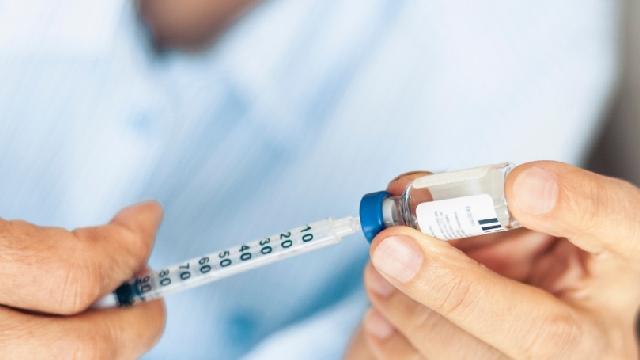
Type 2 diabetes and insulin
What does it mean if you have to take insulin if you have type 2 diabetes?

Using an insulin pump
Find out how insulin pumps work, which ones are available and who qualifies for one on the NHS.

Injecting insulin as an adult - everything you need to know
How and where to inject, insulin pens and avoiding lumps and bumps.

Insulin and children
How to give insulin injections to babies and children and tips to help them do their own injections.
Off