Research funded by us has revealed the transformational impacts Flash glucose monitoring has on blood sugar levels and quality of life for people living with type 1 diabetes. The findings drive home how essential it is that everyone who could benefit from technology is able to access it.
A University of Manchester team led by Dr Lalantha Leelarathna and funded by Diabetes UK, ran a clinical trial to learn if second-generation Flash (FreeStyle Libre 2) tech is better than finger-prick testing for people living with type 1 diabetes. The findings were first announced earlier this year at our Professional Conference and today they’ve been published in the New England Journal of Medicine.
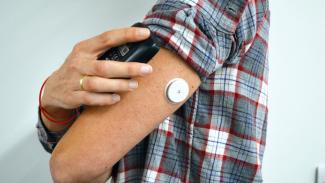
Flash allows people to see what their blood sugar levels are doing minute-by-minute by scanning a smartphone or reader over a sensor. It will also alert people when their levels are going too low or too high.
156 people living with type 1 diabetes from across the UK took part in the trial. Everyone who took part had blood sugar levels above target range. For 24 weeks, half of the participants checked their blood sugar with Flash and the other half carried on using finger prick testing. At the start of the study both groups had similar HbA1c levels.
After 24 weeks:
- Participants using Flash had reduced their HbA1c from an average of 71.6 mmol/mol (8.7%) to 62.7 mmol/mol (7.9%), a decrease of 8.9 mmol/mol (0.8%). Lowering HbA1c by this amount can decrease the risk of developing diabetes complications in the future by up to 40%.
- In comparison, those using finger-prick tests had reduced their HbA1c on average by only 2.2 mmol/mol (0.2%).
- Flash users spent an extra 120 minutes each day with blood sugar levels in the target range (between 3.9 and 10 mmol/L) and 43 minutes less time per day with dangerously low levels (below 3.9 mmol/L).
- Using the technology also helped to reduce the day-to-day burden and emotional strain of living with type 1 diabetes. Participants in the Flash group reported they were happier with their diabetes treatment and that using the technology improved glucose monitoring satisfaction.
Importantly these improvements were seen without an increase in the amount of insulin people used. This suggests Flash helped people to adjust their insulin and make decisions that led to the positive effects on their blood sugar levels.
The fight for Flash
Flash glucose monitoring technology was first made available through the NHS in 2017. Currently, more than half of people living with type 1 diabetes are prescribed Flash on the NHS in England. In March 2022, the National Institute of Health and Care Excellence (NICE) recommended Flash or other continuous glucose monitoring for use in all adults with type 1 diabetes, and Flash for some people with type 2 diabetes who have two or more insulin injections a day.
Dr Elizabeth Robertson, Director of Research at Diabetes UK, said:
“This study confirms the radical improvements Flash can bring to the lives of people living with type 1 diabetes, helping them to reduce their blood glucose levels – protecting against short and long-term diabetes complications – and removing some of the relentless burden of managing the condition.
“It is crucial that everyone who is eligible for this transformative technology is able to access it. Following NICE’s recommendation of Flash or CGM for all adults with type 1 diabetes, these results are a reminder of the benefits of this innovative technology, driving home the importance of equitable access to this life-changing intervention across the UK.”
Dr Lalantha Leelarathna said:
“Ability to monitor glucose without painful finger-sticks is life-changing for many people living with type 1 diabetes. With the use of second generation intermittently scanned continuous glucose monitoring, we found significant improvements in average glucose levels and a reduction in both high and low glucose levels, helping people to spend more time with normal glucose levels. Further treatment satisfaction and glucose monitoring satisfaction was also higher in those using glucose sensors. We call for universal funding of this life changing technology for all people living with type 1 diabetes across the world. Further work is underway to assess the cost-effectiveness of this technology.”
These findings help to demonstrate why Flash technology should be a standard part of diabetes management for everyone who could benefit, not just an added luxury. Widening access to diabetes tech for more people living with all types of diabetes will mean happier and healthier lives.
