Knowing your blood sugar levels helps you manage your diabetes and reduces your risk of having serious complications – now and in the future.
On this page:
- What are blood sugar levels?
- Can I check my own blood sugar levels?
- Why test blood sugar levels?
- How to check your blood sugar levels
- HbA1c test
- What are healthy blood sugar levels for my target range?
- What if my blood sugar levels are too low?
- What if my blood sugar levels are too high?
What are blood sugar levels?
Your blood sugar levels, also known as blood glucose levels, are a measurement that show how much glucose you have in your blood.
Glucose is a sugar that you get from food and drink. Your blood sugar levels go up and down throughout the day and for people living with diabetes these changes are larger and happen more often than in people who don't have diabetes.
Can I check my own blood sugar levels?
You can do blood sugar level check by doing a finger-prick test, or by using an blood sugar monitor called a continuous glucose monitor (or CGM). You can do this several times a day – helping you keep an eye on your levels as you go about your life and help you work out what to eat and how much medication to take.
Not everyone with diabetes needs to check their levels like this. You’ll need to if you take certain diabetes medication. Always talk to your healthcare team if you’re not sure whether that’s you – they’ll give you advice on whether to check them yourself and how often.
And there’s also something called an HbA1c, which is a blood test to measure your average blood sugar level over the last three months. Everyone with diabetes is entitled to this check.
High blood sugar levels increase your risk of developing serious complications. However you manage your diabetes, stay in the know about your blood sugar levels
Why test blood sugar levels?
If you take certain medication, like insulin or sulphonylureas, checking your blood sugar levels is a vital part of living with diabetes. It can help you work out when you need to take more medication, when you need to eat something or for when you want to get up and move around more.
Routine checks can help you know when you might be starting to go too low (called a hypo) or too high (called a hyper). It’s a way of getting to know your body and how it works. It can help you and your healthcare team spot patterns too. Do you write your results down? You might find that helpful.
But importantly, it will help you stay healthy and prevent serious diabetes complications now and in the future. By complications, we mean serious problems in places like your feet and your eyes. This happens because too much sugar in the blood damages your blood vessels, making it harder for blood to flow around your body. This can lead to very serious problems like sight loss and needing an amputation.
The higher your blood sugar levels are and the longer they’re high for, the more at risk you are.
Monitors like CGMs are available for purchase for people without diabetes but it is important to note these cannot be used to diagnose diabetes or prediabetes. Diagnosis can only be done by blood tests, which your GP can arrange.
There is also currently very little published evidence on the use of CGM in people without diabetes, so people need to be careful when relying on such results to make decisions about health.
We are not in a position to advise on CGM use in people without diabetes and recommend people speak to the providers of their device for further information.
How to check your blood sugar levels
Continuous glucose monitors
More and more people with diabetes are choosing to use a CGM to check their blood sugar levels.
Continuous glucose monitoring means that you can check your blood sugar levels without needing to prick your finger. You wear a small sensor on your body day and night that reads your blood sugar levels so you can see your levels on your mobile phone or another device called a reader. If you use FreeStyle Libre 2 Plus sensors you can also scan the sensor with the reader.
But continuous glucose monitoring doesn’t measure the sugar in your blood. It measures the amount of sugar in the fluid surrounding your cells, called interstitial fluid.
It’s not quite as accurate as a finger prick test as it lags behind blood sugar levels by up to 15 minutes. And the difference between blood sugar levels and CGM readings is more likely to be greater when you’re eating or exercising.
Even if you’re offered a CGM by your healthcare team, it’s important that you still get a blood glucose meter on prescription to let you do finger prick checks.
Find out if you're eligible for a free CGM on the NHS.
Finger-pricking
This is how you find out what your blood sugar level is at that moment in time. It’s a snapshot.
Your healthcare team will show you how to do the test and it’s important that you’re taught how to do it properly – otherwise you could get the wrong results.
For some people, finger-prick testing isn’t a problem and it quickly becomes part of their normal routine. For others, it can be a stressful experience, and that’s totally understandable. Knowing all the facts and speaking to other people can help – contact our helpline or chat to others with diabetes on our online forum. They’ve been through it too and will understand your worries.
Watch our video and follow our simple steps on how to test your blood sugar levels in the right way and safely.
We have more information for you if your child has diabetes and you’re checking their blood sugar levels for them.
You’ll need these things to do the test:
- a blood testing meter
- a finger prick device and lancet
- some test strips
- a sharps bin, so you can throw the needles away safely.
If you’re missing one of these, speak to your healthcare team.
Blood testing meters
New meters come on the market all the time, so it can be tricky choosing the right one. It’s best to ask your healthcare team for advice on a meter that’ll suit you.
If you have sight problems, you may not be able to use some meters so your healthcare team can suggest alternatives.
Some people can get meters on prescription. But if you choose to buy your own meter, you might not get a prescription for the test strips it uses. Chat to your healthcare team.
Finger-prick devices and lancets
Finger-prick devices pierce the skin with a needle so that a drop of blood can be taken for testing. The needle is called a lancet.
You can adjust the device to change how far it goes into the skin. It’ll depend on the thickness of the skin.
Lancets come in different sizes and thicknesses (or gauges). A higher-gauge lancet is thinner so is normally less painful, but it might not always give you enough blood.
You can only use a lancet once or they get blunt and are painful to use.
Test strips
Test strips usually come in batches of 50 and must work with the type of meter you’ve chosen.
If you are refused test strips, take it up with your GP practice. If that doesn’t work, contact your local Clinical Commissioning Group (your local CCG manages the NHS Trust in your area).
If you decide to buy strips from outside the UK or online, you’ll need to check they’re adjusted to UK specifications.
How to do a finger-prick test
{"preview_thumbnail":"/s3/files/styles/video_embed_wysiwyg_preview/public/video_thumbnails/NUskHl7APHE.jpg?itok=IohnqDw9","video_url":"https://www.youtube.com/watch?v=NUskHl7APHE","settings":{"responsive":1,"width":"854","height":"480","autoplay":0},"settings_summary":["Embedded Video (Responsive)."]}
Your healthcare team will show you how to do it the first time, but these are the key steps:
- Wash your hands with soap and warm water. Don’t use wet wipes as the glycerine in them can affect the test result. Make sure your hands are warm so it’s easier to get blood and won’t hurt as much.
- Take a test strip and slot it into the meter to turn it on. Some meters will have tests strips built in.
- Remove the cap from your finger prick device and put in a new lancet. Then put the cap back on and set the device by pulling or clicking the plunger.
- Choose which finger to prick but avoid your thumb or index finger (finger next to your thumb). And don’t prick the middle, or too close to a nail. Place the device against the side of your finger and press the plunger. Use a different finger each time and a different area.
- Take your meter with the test strip and hold it against the drop of blood. It’ll tell you if the test strip is filled, usually by beeping.
- Before you look at your reading, check your finger. Use a tissue to stop bleeding, then use it to take out the lancet and throw it away in your sharps bin.
- By this time, your meter will probably show the result. Note it down.
- You can use the same tissue to take out the test strip and throw that away too. Taking out the strip will usually turn the meter off.
HbA1c test
As well as regularly testing your own blood sugar levels, at least once a year your healthcare team will ask you to come in for an HbA1c blood test. This checks your average blood sugar levels over the last three months and helps your diabetes team and you spot trends over time.
This is one of your essential diabetes health checks and it’s really important you understand what your results mean. A high HbA1c means you have too much sugar in your blood. This means you’re more likely to develop diabetes complications, like serious problems with your eyes and feet. So it's really important to have this test regularly so that you can make changes and reduce your risk of getting complications.
We’ve got more information about the HbA1c test and what your levels mean.
Make a note of your readings
It may sound obvious, but you must record your readings. Note them down in a diary, a notebook or in your phone calendar. Some meters have software that lets you do this. You could try a diabetes app too.
You and your healthcare team can then look back over your results to see if you need to adjust your treatment.
What are healthy blood sugar levels for my target range?
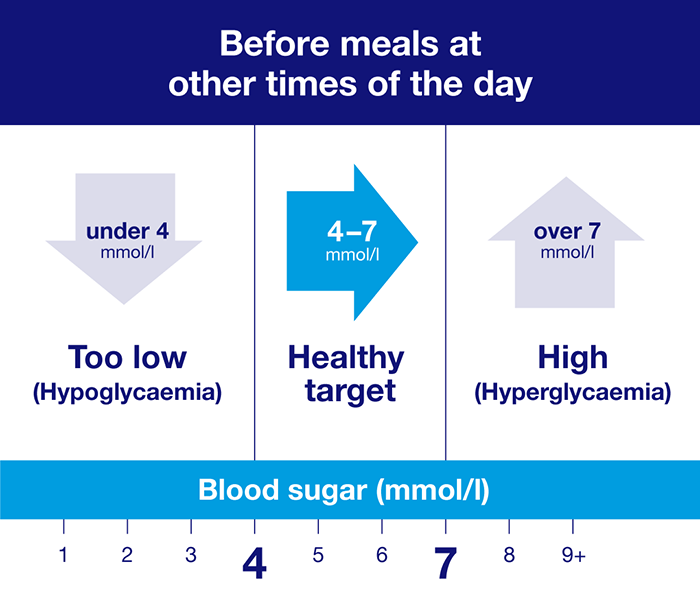
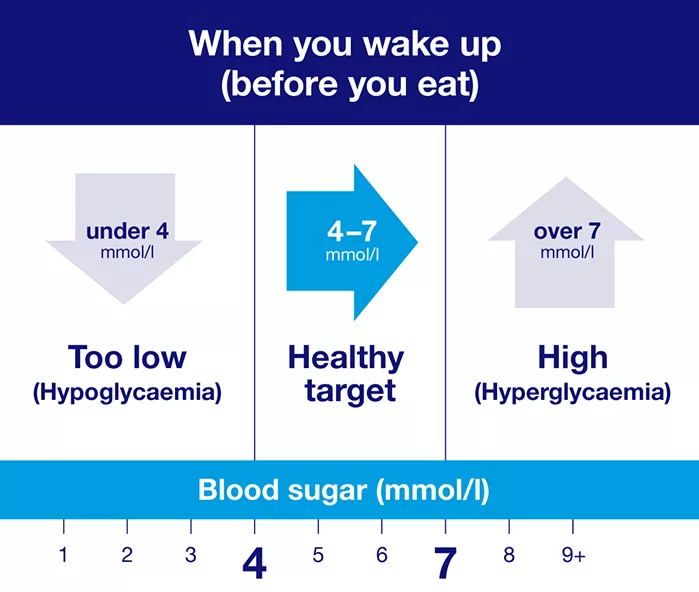

These are general blood sugar level targets for adults living with diabetes. Your individual targets may differ.
You might be asking, what's the normal range for blood sugar levels? The answer is, there is a healthy range that you should ideally be aiming for. The infographics above show the general guidelines, but your individual target range for your blood sugar levels may be different. Your healthcare team will agree with you what it is.
You’ll get different readings at different times of the day, depending on things like what you’ve eaten and how much you are moving around. Blood sugar levels are measured in mmol/l, which stands for millimoles per litre.
Here’s a guide to help you get started on finding your target range:
If you’re a child with type 1 diabetes:
- when you wake up and before meals: 4 to 7mmol/l
- after meals: 5 to 9mmol/l
If you’re an adult with type 1 diabetes:
- when you wake up and before meals: 5 to 7mmol/l
- before meals at other times of the day: 4 to 7mmol/l
- after meals: 5-9mmol/l at least 90 minutes after eating
A bedtime target should be agreed with you by your healthcare team too.
If you have type 2 diabetes:
-
There are currently no NICE recommendations for these type of blood sugar targets if you have type 2 diabetes. If you live with type 2 diabetes it’s important that you speak to your healthcare team about your individual blood sugar targets. You can read our HbA1c page to learn about HbA1c targets in type 2 diabetes, and our Time in Range page to learn more about target ranges.
Pregnant women with any form of diabetes, including gestational diabetes:
- Fasting: below 5.3mmol/l
- One hour after meals: below 7.8mmol/l
- If you’re not able to check until two hours – rather than one hour – after a meal, you should aim for below 6.4mmol/l
- Pregnant women should keep blood sugar levels above 4 mmol/l
And remember your individual target range for your blood sugar levels may be different. Your healthcare team will agree with you what it is and help you reach these targets, so you can reduce the risks for you and your baby.
We have lots more information to help you if you’re planning to have a baby or you’re pregnant now.
What happens when your blood sugar levels are too low?
If your blood sugar levels are too low, usually below 4 mmol/l, you may experience a hypo. Hypos need to be treated immediately, otherwise your blood sugar levels will drop further. If this happens, you may experience a severe hypo and need emergency treatment.
There are many different symptoms of a hypo, so it’s important that you are aware of the signs in case your blood sugar level gets too low. We’ve also got more information about what to do if you are having a hypo.
What happens when your blood sugar levels are too high?
If your blood sugar levels are slightly above your targets, there are usually no symptoms. But if your blood sugar levels become too high, you may experience some symptoms associated with a hyper.
The blood sugar level at which symptoms begin to appear is different for everyone, but the common symptoms include passing more urine than normal, being very thirsty, having headaches and feeling tired and lethargic.
It’s important that you know how to treat a hyper to avoid developing ketones in the blood.
