This guide is for healthcare professionals working with people with Type 1 and Type 2 diabetes who are experiencing emotional difficulties. It offers strategies and tools for how to recognise and have conversations about emotional problems, as well as for providing appropriate support.
This guide was originally developed by the Australian Centre for Behavioural Research in Diabetes (ACBRD), the National Diabetes Services Scheme (NDSS) and Diabetes Australia in 2016, which is available to download from the NDSS website. The UK edition (2019) of these guidelines were produced by Diabetes UK under a royalty-free, UK only, non-exclusive sub-license from Diabetes Australia.
Download the Diabetes and emotional health guide (PDF, 3MB)
You can find all the author acknowledgements, references, appendices, questionnaires and more in the full PDF guide.
For more information on language and diabetes, download the NHS England guide, Language Matters (PDF, 315KB) or at ‘Language Matters Diabetes’, which showcases the worldwide Language Matters documents.
Contents
- Introduction to the guide
- Who this guide is for
- How to use this guide
- Leaflets for people with diabetes
- 7As model - what is it and how does it work?
- Chapter 1 – Communication and engagement
- Chapter 2 – Facing life with diabetes
- Chapter 3 – Diabetes distress
- Chapter 4 – Fear of hypoglycaemia (and other diabetes-specific fears)
- Chapter 5 – Psychological barriers to insulin use
- Chapter 6 – Depression
- Chapter 7 – Anxiety disorders
- Chapter 8 – Eating problems
- Chapter 9 – Referring to a mental health professional
Introduction to the guide
Diabetes self-management is demanding and complex. Activities such as monitoring blood glucose, injecting insulin, taking oral medications, regular physical activity, and healthy eating all require a comprehensive understanding of diabetes, as well as healthy coping, and skills in problem-solving and risk reduction. Diabetes is more than a physical health condition, it has behavioural, psychological, and social impacts, and demands high levels of self-efficacy, resilience, perceived control, and empowerment. Thus, it is unsurprising that living with diabetes negatively impacts upon the emotional well-being and quality of life of many people living with the condition.
Emotional and mental health problems (collectively referred to as psychological problems from here on), such as diabetes distress and depression, are common among adults with diabetes and are associated with sub-optimal self-management, diabetes-related complications, reduced quality of life, and increased health care costs. As noted by Jones and colleagues: ‘maintaining or achieving good psychological well-being and quality of life is an important outcome of diabetes care in its own right.’ This sentiment is shared by people with diabetes and health professionals, who recognise emotional health to be an important component of standard diabetes care.
Why is this guide needed?
‘We must move beyond the tendency to place an artificial divide between the emotional and the physical aspects of diabetes management that can lead to labelling the emotional aspects of diabetes a pathological condition. The two are so intertwined and interrelated that simply calling the emotional side a co-morbidity is counterproductive.’(Lawrence Fisher, Jeffrey Gonzalez and William Polonsky)
Given that separating psychological care from the context of diabetes self-management is rarely easy nor desirable, there is a strong argument that basic psychological care needs to be incorporated into diabetes care pathways, including assessment and treatment of the psychological problems frequently faced by people with diabetes. International guidelines reflect this view; recommending awareness and assessment of psychological problems in diabetes clinical practice.
Furthermore, the need for mental health care for people with diabetes is acknowledged in many of the UK National Diabetes Strategies, although often limited to anxiety and depression diagnoses.
Despite the numerous guidelines, and recognition by health professionals and Governments, the emotional and mental health needs of people with diabetes are often undetected and unmet in clinical practice. Furthermore, there is little evidence to demonstrate significant progress in the implementation of such recommendations. Health professionals cite lack of skills, confidence, time, and limited access to practical resources as common barriers. Whilst existing guidelines acknowledge the importance of psychological problems in diabetes and some make recommendations for assessing them, most fall short in providing guidance about how to incorporate this into the daily clinical practice setting. This guide is designed to complement and facilitate the implementation of existing guidelines.
The aim of this guide is to promote awareness of, and communication about, psychological problems affecting adults with diabetes. The objectives are to:
- raise awareness among health professionals of the prevalence and consequences of psychological problems among adults with diabetes
- provide a set of practice points for how to identify, communicate about, and address psychological problems with adults with diabetes in clinical practice
- foster skills development among health professionals for communicating about psychological problems in diabetes care, by providing examples of questions and responses, with case studies to demonstrate their implementation
- provide the practical tools (e.g. questionnaires, information leaflets, and other resources) to support health professionals in this endeavour
What do national and international guidelines say about emotional and mental health?
Guidelines for both Type 1 and Type 2 diabetes clinical care
Commissioners and service providers should work together to ensure emotional and psychological support for people with diabetes of all ages is embedded in each step of the diabetes care pathway and is not limited to people with ‘diagnosable/classifiable’ psychological problems” (Diabetes UK, 2018)
“Provide psychological assessment and appropriate treatment for service users with diabetes and identified mental health issues, such as anxiety or depression” (NHS Right Care for Diabetes, Core Service Component 9, 2018)
“Providers should consider an assessment of symptoms of depression, anxiety, and disordered eating, and of cognitive factors using patient-appropriate, validated tools at the initial visit, at periodic intervals and when there is a change in disease, treatment or life circumstance.”
“Routinely monitor people with diabetes for diabetes distress, particularly when treatment targets are not met and/or at the onset of diabetes complications.”
“Psychosocial care should be integrated with a collaborative, patient-centered approach and provided to all people with diabetes, with the goals of optimizing health outcomes and health-related quality of life.” (American Diabetes Association, 2019)
“Screening for depression should be performed routinely for adults with diabetes because untreated depression can have serious clinical implications for patients with diabetes.”
“Patients with depression should be referred to mental health professionals who are members of the diabetes
care team.” (American Association of Clinical Endocrinologists and American College of Endocrinology, 2015)
“Individuals with diabetes should be regularly screened for subclinical psychological distress and psychiatric disorders (e.g. depressive and anxiety disorders) by interview or with a standardized questionnaire.”
“Psychosocial interventions should be integrated into diabetes care plans.” (Canadian Diabetes Association, 2013)
Guidelines for Type 1 diabetes clinical care only
“Members of professional teams providing care or advice to adults with Type 1 diabetes should be alert to the development or presence of clinical or subclinical depression and/or anxiety, in particular if someone reports or appears to be having difficulties with self-management.” (National Institute for Health and Care Excellence, 2015)
“Regular assessment of a broad range of psychological and behavioural problems in… adults with Type 1 diabetes is recommended… this should include anxiety, depression and eating disorders.”
“…refer those with significant psychological problems to services or colleagues with expertise in this area.” (Scottish Intercollegiate Guidelines Network, 2010)
Guidelines for Type 2 diabetes clinical care only
“Annually: patients with diabetes can be assessed for mental health issues, social isolation/networks and family or work stress. Consider assessing diabetes distress through the use of the PAID questionnaire and depression with the Patient Health Questionnaire-2 (PHQ-2).”
“Referral when appropriate to: psychologist – if issues identified, such as adjustment disorder, depression and/or anxiety.” (Royal Australian College of General Practitioners, 2014)
“Explore the social situation, attitudes, beliefs and worries related to diabetes and self-care issues. Assess well-being (including mood and diabetes distress), periodically, by questioning or validated measures (e.g. WHO-5). Discuss the outcomes and clinical implications with the person with diabetes, and communicate findings to other team members where appropriate.”
“Counsel the person with diabetes in the context of ongoing diabetes education and care. Refer to a mental health-care professional with a knowledge of diabetes when indicated.” (International Diabetes Federation, 2012)
Guidelines for Type 2 diabetes clinical care (of older adults only)
“Screening for and monitoring of depressive symptoms in older people with diabetes should be performed at diagnosis, be an integral part of standard diabetes care, and be part of the annual review.” (International Diabetes Federation, 2013)
What does this practical guide offer?
"I’m really excited... it’s really important and if any health professional reads even any chapter of it [the handbook], I think they’ll come away with a lot more depth and understanding of what it’s like to live with diabetes." - Person with diabetes who was involved in developing the original Australian edition
This guide is an evidence-based, clinically informed, practical resource to support health professionals in meeting the emotional and mental health needs of adults with diabetes. While the guide is informed by evidence, it is not an evidence-based guideline. As recommendations for routine monitoring of emotional well-being have existed in guidelines for 25 years,17 there is little evidence that producing yet another guideline would benefit people with diabetes.
The original Australian edition (2016) of the handbook, on which the UK practical guide (2019) is based, was developed by a team with expertise in psychology and diabetes. Their work has been overseen by a multidisciplinary Expert Reference Group. The guidelines were also peer-reviewed by academic and clinical experts with relevant expertise, and by end users (people with diabetes and health professionals). We acknowledge all those involved in the full PDF guide (3MB).
Who this guide is for
This guide is expected to support health professionals working with adults with Type 1 or Type 2 diabetes.
In many instances it is appropriate to refer to Type 1 and Type 2 diabetes separately. However, for readability purposes, and because research studies often do not separate the two types, we refer to people with diabetes collectively in many parts of the guide. Where a research study has definitively specified the type of diabetes, we have also made the distinction.
Such health professionals include: general practitioners (GPs), specialist and primary care nurses, dietitians, diabetologists, and other health professionals supporting adults with diabetes. Mental health professionals including psychologists, psychiatrists, mental health nurses, and social workers may also find this guide to be a useful resource.
Thus, this guide has been written in a general format that can be adapted to individual needs and circumstances, and it can be used in many ways, depending on your level of knowledge, expertise, setting, and available time.
What is the scope of the guide?
The practice points in this guide have been developed for use specifically with adults with Type 1 or Type 2 diabetes, in the context of the UK healthcare setting.
The scope of this guide does not extend to:
- Children and adolescents with Type 1 or Type 2 diabetes, as the advice may not be appropriate to their developmental stage.
- Adults with other types of diabetes (e.g. gestational, MODY, LADA). It may be appropriate to apply parts of this guide but we advise you to use your professional judgement before doing so.
- People with language, cultural, cognitive, health literacy, or other barriers. It is beyond the scope of this guide to provide specific recommendations for each of these diverse groups, and for many groups the evidence base relating to mental health and diabetes is sparse. Where relevant resources exist these are noted in the chapter. In the absence of evidence specific to these groups, it may be reasonable to extrapolate from this guide and use your professional judgement.
Furthermore, we emphasise the importance of tailoring your approach to the needs of the person – this applies to all people with diabetes, not just those from diverse groups. Throughout this guide, we make suggestions for words you might say, or strategies you might use to address psychological problems. Be guided by the suggestions but avoid using them as a checklist. Reflect upon how relevant the suggestion is for each individual, and tailor your approach to their priorities and preferences.
What are the expected outcomes of the guide?
The overall purpose of this guide is to enhance opportunities for people with diabetes to talk about their emotional well-being with their health professionals and, if problems are present, to identify and address these. This conversation informs a shared decision about appropriate management strategies. It is an important and positive step toward holistic healthcare. We expect the following outcomes:
- Health professionals will feel supported, confident and skilled to: ‘have the conversation’ about emotional and mental health generally or, specifically, how diabetes is impacting upon the person’s emotional well-being, address psychological problems that are within their skillset and remit, and make referrals to specialist care providers, as needed
- People with diabetes will appreciate that their health professionals ask about how diabetes is impacting upon their emotional well-being, and that they are offered support to address identified psychological problems.
- Health professionals and health services will approach psychological problems in diabetes in a consistent and systematic way.
- Emotional and mental health will be integrated into routine diabetes consultations as part of ‘usual care’.
- People with diabetes will be active participants in a person-centred approach to care for their psychological problems.
Organisational culture and considerations
This guide focuses on the skills and resources of the individual health professional, but most work in teams rather than in isolation. We recognise that the service, practice or department you work in may influence your capacity to implement the practices recommended in this guide. However:
"Change will not come if we wait for some other person or some other time. We are the ones we’ve been waiting for. We are the change that we seek." - Barack Obama
You can be the agent of change in your healthcare setting by implementing the following actions to promote holistic care:
- Model the behaviours you would like to see in others; you can be an example to others in your service, practice, or department by demonstrating that psychological problems are at least as important as other aspects of diabetes care.
- Ensure all staff have access to this practical guide
- Provide opportunities for all staff to enhance their communication skills using a person-centred approach.
- Arrange ongoing training for staff relating to psychological problems and diabetes.
- Actively support supervision and mentoring to build skills in addressing psychological problems in people with diabetes.
- Support junior staff to observe discussions about psychological problems and diabetes, and help them review and reflect on the care they provide.
- Incorporate an holistic approach to diabetes care in staff position descriptions, staff induction programmes and staff performance reviews.
How to use this guide
This guide includes information about emotional problems that may be experienced by adults with diabetes. Designed for health professionals working with people with diabetes, it offers strategies and tools for how to recognise and have conversations about emotional problems, as well as for providing appropriate support.
There are nine chapters:
- Chapter 1: Communication and engagement
- Chapter 2: Facing life with diabetes
- Chapters 3 to 8: each focuses on an emotional problem experienced by adults with diabetes
- Chapter 9: Referring to a mental health professional.
There are three appendices:
- Appendix A: Peer support opportunities for people with diabetes, which are also available on each chapter.
- Appendix B: Examples of strategies to address diabetes distress
- Appendix C: Examples of strategies for overcoming psychological barriers to insulin use.
Find all three appendices in the full PDF guide (3MB).
We also reference NHS Language Matters, which you can also download as a PDF (315KB).
This guide has been written with a multidisciplinary audience in mind. Therefore, the format has been developed for the reader to use according to their own needs, knowledge, expertise, setting, and available time. You may choose to:
- read everything, to gain an in-depth understanding
- read the key messages and practice points, then read the relevant detailed sections of the guide as you need them
- dip in-and-out of the specific sections on a need-to-know basis.
Structure of chapters
Chapters 1 and 2 provide background information on communication and engagement, as well as on the experience of diagnosis and how the health professional can best support a person at this time.
As Chapters 3 to 8 focus on specific emotional problems, they are all presented in a similar structure to make it easier for you to navigate the content and find the information you need.
'How common' stats
An estimate of how common the emotional health problem is among people with diabetes. The symbols indicate an approximate proportion of people with diabetes who might be expected to be experiencing the emotional problem (e.g. one in five adults with insulin-treated Type 2 diabetes experience diabetes distress). Underneath the symbols are descriptions of the population to whom the statistic applies. Typically, this refers to three groups: people with Type 1 diabetes, people with Type 2 diabetes who use insulin, and people with Type 2 diabetes who do not use insulin. These estimates are based on the best evidence available. Keep in mind that your own clinic population may vary from the study population in terms of demographic and clinical characteristics. This information is intended as a guide only.
Case studies
Examples of how the 7 As model can be applied in clinical practice. Keep in mind that they are illustrative; they are not applicable to, nor representative of, every person or circumstance. In each case, the content is a snapshot of a conversation, for example, to demonstrate how to ask questions or introduce the use of a questionnaire.
The characters in the case studies are fictional, though the content of their stories have been inspired by clinical practice.
Acronyms and abbreviations
- 7 As Aware, Ask, Assess, Advise, Assist, Assign, Arrange
- BMI Body Mass Index
- CBT Cognitive Behavioural Therapy
- CBT-E Enhanced Cognitive Behavioural Therapy
- DAFNE Dose Adjustment for Normal Eating
- DDS Diabetes Distress Scale
- DEPS-R Diabetes Eating Problem Survey – Revised
- DESMOND Diabetes Education and Self-Management for Ongoing and Newly Diagnosed
- DOC Diabetes Online Community
- DSM-5 Diagnostic and Statistical Manual of Mental Disorders, fifth edition
- GAD-2 Generalised Anxiety Disorder (questionnaire); two-item version
- GAD-7 Generalised Anxiety Disorder (questionnaire); seven-item version
- GBDOC Great Britain Diabetes Online Community
- GP General Practitioner
- HbA1c Haemoglobin A1C
- HFS-II W Hypoglycaemia Fear Survey version two: Worry Scale
- ICD-10 International Statistical Classification of Disease and Related Health Problems, 10th revision
- ITAS Insulin Treatment Appraisal Scale
- JDRF Juvenile Diabetes Research Foundation
- mSCOFF Modified SCOFF
- PAID Problem Areas in Diabetes (scale)
- PHQ-2 Patient Health Questionnaire; two-item version
- PHQ-9 Patient Health Questionnaire; nine-item version
- SPIKES Setting up, Perception, Invitation, Knowledge, Emotions, Strategy and summary
- SSRIs Selective Serotonin Re-uptake Inhibitors
- WHO-5 World Health Organization Well-being Index Five (questionnaire)
7As model
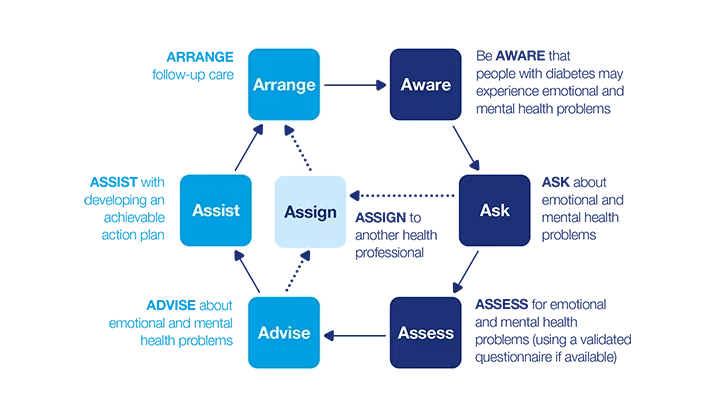
A key feature of these guidelines are a practical 7As model. This dynamic model describes a seven-step process that can be applied in clinical practice as part of a person-centred approach. Find out more about the 7As, what they are and how they work.
You can also download summary sheets of the 7As model (PDF, 352 KB)
Leaflets for people with diabetes
Each leaflet focuses on a specific psychological problem, corresponding with the guide chapters. The leaflets include tips and resources that people with diabetes may find helpful. They can be used in various ways:
- keep copies in your clinic waiting room where people with diabetes can access them easily
- use a copy to facilitate a conversation about emotional health
- give a copy to the person to take home with them after having a conversation about an emotional health problem.
Download our leaflets for people with diabetes:
- Adjusting to life with diabetes (PDF, 44KB)
- Diabetes and anxiety (PDF, 47KB)
- Depression and diabetes (PDF, 45KB)
- Diabetes distress (PDF, 42KB)
- Eating problems and diabetes (PDF, 45KB)
- Fear of hypos (PDF, 44KB)
- Peer support and diabetes (PDF, 39KB)
- Worries about insulin (PDF, 42KB)
See Diabetes and emotional health PDF (3MB) for our full list of references.
Disclaimer: Please note you may find this information of use but please note that these pages are not updated or maintained regularly and some of this information may be out of date.
